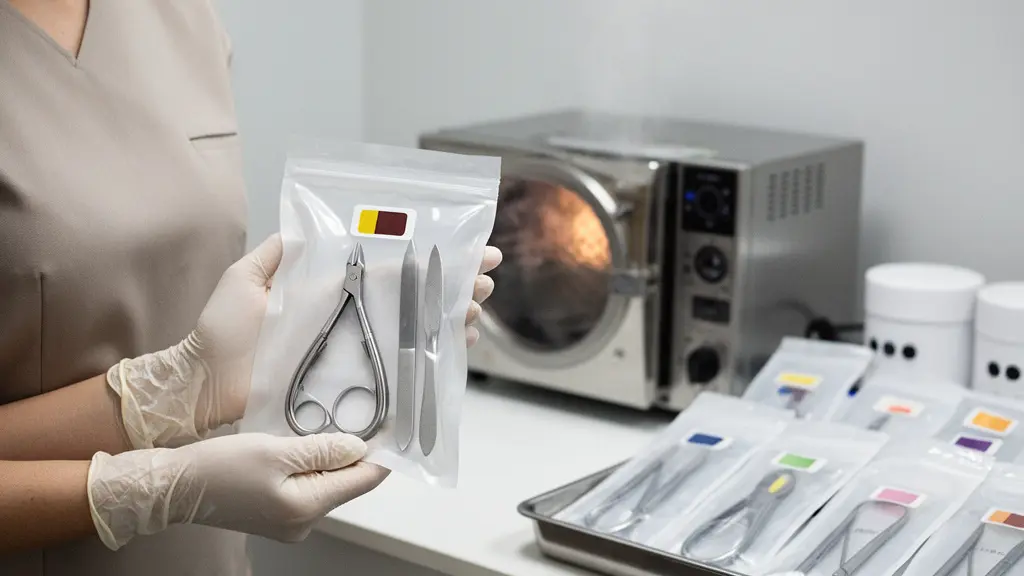
Compliance is not just about cleanliness; it is about the verifiable proof of that cleanliness through rigorous documentation.
- A valid sterilization log must track date, cycle type, and specific chemical indicator results for every single load.
- Visual cleanliness is insufficient; state boards require biological indicators and documented contact times.
Recommendation: Audit your current logbook against the specific data points listed in this guide to close liability gaps immediately.
Many salon owners operate under the dangerous assumption that simply buying an autoclave and using blue liquid guarantees safety. They believe that if the tools look clean, the inspector will be satisfied. This mindset is the primary cause of fines and license suspensions. While facettes like gem application or intricate nail art draw clients in, the backbone of your business is the unglamorous reality of infection control. A lack of visible debris is not the same as sterility.
However, the real vulnerability in most salons isn’t the cleaning process itself, but the lack of an evidentiary trail. What if the key to passing an inspection wasn’t just the temperature of your machine, but the precision of your pen? Documentation is the only defense against liability. Without a logs entry that traces a specific tool to a specific sterilization cycle, legally, that tool is dirty. This guide shifts the focus from hygiene theater to forensic-level compliance.
We will dissect the exact logging protocols, the physics of porous tools, and the specific paperwork required to turn your safety measures into an impenetrable legal shield.
The following structure outlines the critical compliance clusters required to secure your establishment against regulatory scrutiny.
Table of Contents: Navigating Sterilization Compliance
- Pouches and Indicators: How to Prove the Tools Are Sterile?
- Pumice Stones and Buffers: Why You Must Throw Them Away?
- The 10-Minute Protocol: How to Disinfect Jets Between Clients?
- How to Explain Your Sanitation Fee to Price-Sensitive Clients?
- N95 vs. Surgical Masks: What Filters Nail Dust Effectively?
- The Blue Liquid Myth: Is Barbicide Actually Effective If Not Changed?
- What Are the Instant-Fail Violations During a State Board Inspection?
- How to Spot a “Chop Shop” Salon Before You Even Sit Down?
Pouches and Indicators: How to Prove the Tools Are Sterile?
An autoclave without a log is simply a pressure cooker. To a health inspector, the sterilization process does not exist unless it is recorded with forensic accuracy. The common error is treating the logbook as a general attendance sheet rather than a specific chain of custody for your instruments. You must establish a direct link between the physical pouch used on a client and the specific machine cycle that sterilized it.
This proof relies on visual indicators. A color change on a pouch confirms heat exposure, but it does not guarantee sterility. This is why distinguishing between external and internal indicators is a non-negotiable aspect of your protocol.
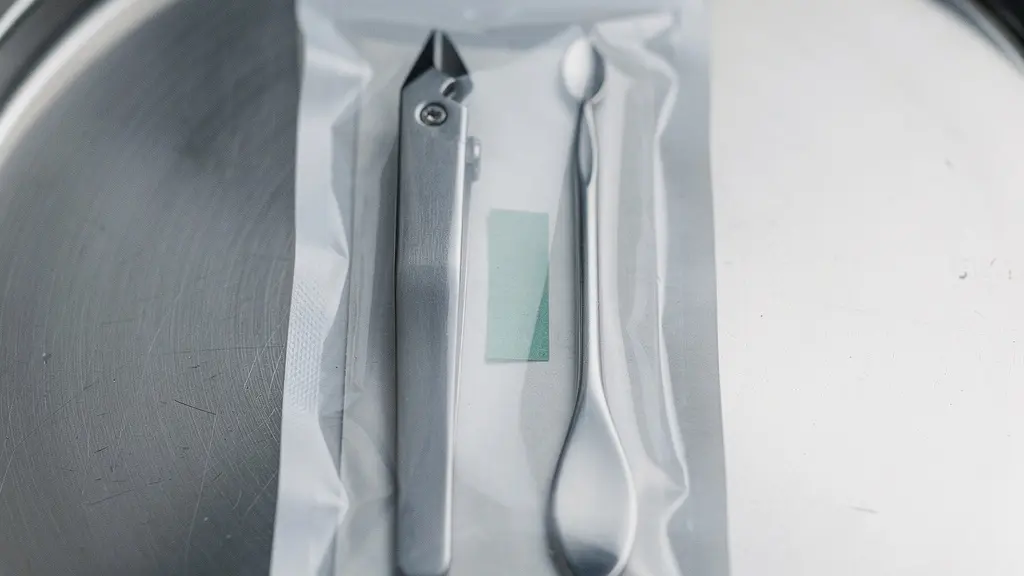
As illustrated above, the internal strip is the critical witness; it proves steam penetrated the packaging. However, the physical evidence must be backed by data. Regulatory bodies dictate a precise workflow for validation. For instance, protocols require that you record the date, sterilizer identification, and cycle type for every run, alongside the specific result of the chemical indicator.
Failing to log a single cycle breaks the chain of evidence, rendering the tools legally non-sterile regardless of their physical condition.
Pumice Stones and Buffers: Why You Must Throw Them Away?
The distinction between porous and non-porous materials is the single most frequent point of failure in infection control. Items such as pumice stones, buffers, and wood sticks are structurally incapable of being sterilized. Their microscopic texture creates a sanctuary for pathogens that liquid disinfectants cannot penetrate.
Many salon owners attempt to wash or spray these items to save costs. This is a violation of basic microbiology and state law. If an item is porous, it is single-use. The regulation is binary: if it absorbs liquid, it absorbs bacteria. Regulatory language is explicit on this matter. You must identify which tools and supplies cannot be disinfected and dispose of them immediately after use on a single client.
Case Study: The Cross-Infection Risk of Reused Pumice
Nail industry education bodies have reinforced why pumice stones should never be reused. Due to their inherent porosity, they trap debris and microbes that cannot be reliably removed. The compliant alternative is to utilize non-porous stainless steel handles paired with disposable abrasive pads. This ensures that the only part of the tool touching the client is new, eliminating the transmission vector entirely.
Treating a porous item as reusable is not a money-saving tactic; it is a direct path to a negligence lawsuit.
The 10-Minute Protocol: How to Disinfect Jets Between Clients?
Pedicure basins, specifically those with piped jets, are high-risk zones for biofilm accumulation. The complexity of the internal piping allows bacteria to thrive even when the visible basin surface appears spotless. The “spray and wipe” method is wholly inadequate for these systems.
Compliance here is measured in contact time. A disinfectant must remain wet on the surface for the full duration specified on the manufacturer’s label—typically 10 minutes—to be effective. For circulating spas, this means the system must run with the disinfectant solution circulating through the pipes.

The image above depicts the standard for a reset: drained, cleared of debris, and ready for the timed cycle. Federal guidelines underscore the rigor required. You must apply an EPA-registered hospital disinfectant exactly per label and keep surfaces wet for the full 10 minutes. Shortcuts here are not just regulatory violations; they are public health hazards.
As the Texas Department of Licensing and Regulation (TDLR) states in their inspections guide:
“A record must be kept on a department-approved form… [with] the date and time of each cleaning and disinfecting.”
– Texas Department of Licensing and Regulation (TDLR), Inspections Guide for Barbering and Cosmetology
Ignoring the circulation requirement allows biofilm to colonize the internal plumbing, turning your spa chair into a bacterial incubator.
How to Explain Your Sanitation Fee to Price-Sensitive Clients?
Implementing hospital-grade sterilization protocols incurs significant costs in time, chemistry, and disposable materials. Absorbing these costs erodes margins, yet passing them on can alienate clients if communicated poorly. The challenge is framing the fee not as a surcharge, but as a guarantee of safety.
Clients are often unaware of the invisible labor involved in compliance. When you itemize a “Sanitation Fee,” you must immediately define the value it delivers. It is not an arbitrary tax; it is the cost of single-use files, autoclave pouches, and verified biological testing. Transparency transforms a hidden cost into a competitive advantage.
Research into consumer psychology supports this approach. Studies suggest that reframing an added cost from a ‘surcharge’ to a clear client benefit can significantly reduce customer resistance. By explicitly linking the fee to their personal protection, you shift the narrative from price to value.
A client who understands that the fee pays for their safety is a client who will pay it willingly and return.
N95 vs. Surgical Masks: What Filters Nail Dust Effectively?
The air quality in a nail salon is often compromised by microscopic particulates generated during filing and removal. A common misconception is that a standard surgical mask offers protection to the technician. In reality, surgical masks are designed to protect the patient from the wearer’s droplets, not to filter incoming dust from the wearer’s lungs.
For effective filtration of nail dust and acrylic particulates, a NIOSH-approved N95 respirator is the minimum standard. The fit is paramount; gaps around the nose or chin render the filter useless. This is a matter of long-term occupational health, as chronic exposure to these particulates carries documented risks.
Scientific data reinforces the severity of the exposure. A 2024 study measured mean breathing-zone metal concentrations in nail salons, identifying elements like manganese and lead, which underscores the absolute necessity of proper PPE. While ventilation handles vapors, only a properly fitted respirator handles the heavy metals found in dust.
To ensure protection, follow the fit-check protocol provided by the CDC/NIOSH:
- Step 1: Use a NIOSH-approved filtering facepiece respirator (e.g., N95) for particulates.
- Step 2: Remember that these do not protect against chemical vapors; ventilation is required for that.
- Step 3: Perform a user seal check every single time you don the mask.
- Step 4: Exhale gently while blocking air-exit paths to check for positive pressure buildup.
- Step 5: Inhale quickly while blocking air-entry paths to check for negative pressure collapse.
Relying on a loose-fitting surgical mask for dust protection provides a false sense of security while pollutants bypass the barrier entirely.
The Blue Liquid Myth: Is Barbicide Actually Effective If Not Changed?
The iconic blue disinfectant jar is a staple in salons, but it is often misused as permanent furniture rather than a functional chemical bath. The efficacy of Quaternary Ammonium Compounds (Quats) is not infinite. It degrades rapidly when introduced to organic debris such as skin cells, nail dust, or oils.
A “topping off” habit—adding fresh liquid to old—dilutes the solution and fails to restore its biocidal power. If the liquid is cloudy, it is contaminated and likely ineffective. The strict rule is daily replacement, or immediate replacement upon visible contamination. The chemistry demands a specific ratio of water to concentrate to function; guessing the mixture renders it useless.
Peer-reviewed research confirms that organic matter influenced the biocidal action of disinfectants, with performance dropping significantly in soil-disinfectant interaction tests. This scientific reality mandates a rigorous changing schedule.
Using old, cloudy disinfectant is essentially soaking your tools in a bath of accumulated bacteria.
What Are the Instant-Fail Violations During a State Board Inspection?
Inspections are often pass/fail scenarios based on critical violations. While minor infractions might result in a warning, certain conditions trigger immediate fines or license suspension. These usually revolve around the immediate threat of infection or the inability to inspect the premises.
Understanding the fine schedule highlights the financial risk of negligence. Items like unlicensed personnel or the presence of prohibited tools (like credo blades) are non-negotiable. However, paperwork violations often catch owners off guard. An expired license or a missing logbook are administrative errors with heavy financial penalties.
To audit your salon before the inspector arrives, use this checklist:
Compliance Audit: The First 5 Minutes
- Verify Licenses: Confirm all personnel are licensed and that current licenses are visibly posted.
- Label Containers: Ensure every bottle has a manufacturer label (no mystery fluids).
- Check Waste Controls: Verify waste containers are covered and labelled; liners must be changed daily.
- Audit Single-Use: Confirm no porous items (files, buffers) are being reused or stored with clean tools.
- Separate Tools: Ensure clean tools are covered and strictly separated from used/dirty implements.
The following table illustrates the financial impact of common violations, derived from California regulatory fine schedules:
These penalties accumulate rapidly, as shown in this regulatory fine schedule.
| Violation area | Example regulatory item | 1st | 2nd | 3rd |
|---|---|---|---|---|
| Inspector access | Access to establishment for inspection (BPC 7313) | $250 | $500 | $750 |
| Licensing | Unlicensed establishment (BPC 7317) | $500 | $1,000 | $1,000 |
| Licensing | Unlicensed individual (BPC 7317) | $1,000 | $1,000 | $1,000 |
| License status | Expired establishment license (BPC 7317) | $250 | $300 | $500 |
| Tools / methods | Use of illegal metal instruments (BPC 7320.1) | $250 | $500 | $500 |
| Tools / methods | Illegal treatment methods (BPC 7320.2) | $500 | $500 | $500 |
Proactive self-inspection is the only way to ensure that when the state board walks in, your doors stay open.
Key Takeaways
- Logbooks must link specific tools to specific sterilization cycles for legal validity.
- Porous items are single-use only; reusing them is a primary vector for cross-infection.
- Disinfectants require precise contact time and daily replacement to remain effective.
How to Spot a “Chop Shop” Salon Before You Even Sit Down?
Recognizing the signs of a non-compliant salon—often colloquially termed a “chop shop”—is essential for differentiating your own high-standard business. These establishments prioritize volume over safety, often skipping the expensive and time-consuming steps of proper sterilization. The visual cues are distinct: cluttered stations, unlabeled bottles, and the reuse of disposable items.
One of the most significant indicators involves the chemical composition of the products used. Discount salons may utilize Methyl Methacrylate (MMA), a bonding agent banned in many jurisdictions due to health risks.
Regulatory Action: The MMA Red Flag
California’s Department of Toxic Substances Control has moved to list nail products containing MMA as a ‘Priority Product’ under Safer Consumer Products regulations. The presence of MMA is a major red flag for a “chop shop” operation, signaling a disregard for both worker safety and regulatory compliance. Identifying and excluding such substances is a hallmark of a professional, compliant salon.

The image above contrasts the chaotic, risky environment of a chop shop with the structured, sterile setup of a professional salon. Your goal is to be undeniably on the left side of this image. Compliance is your brand’s most valuable asset.
Audit your logs today, verify your chemical indicators, and ensure your establishment stands as a fortress of safety in an industry often compromised by shortcuts.